Why Some RHT Initiatives Get Funded (and Others Don’t)

Billions of dollars in funding are entering the system through the Rural Health Transformation (RHT) program, yet many rural health leaders are still wondering: Why do some initiatives move forward while others don’t?
The RHT program doesn’t fund technology purchases or operational improvements in isolation, it funds initiatives that demonstrate transformation and measurable outcomes.
Across the country, rural hospitals are dealing with remarkably similar operational challenges: workforce shortages, clinician burnout, aging infrastructure, limited specialty access, outdated technology environments, and more. In many cases, the initiatives hospitals propose to address those challenges also look similar.
And yet, when state transformation programs evaluate proposals, some initiatives advance while others stall.
Understanding why that happens is becoming increasingly important as new funding opportunities continue to emerge. It could very well mean the difference between your proposal securing funding… or ending up in the trash.
Two Similar Submissions. Different Outcomes.
Two rural hospitals are pursuing a similar goal: improving clinician efficiency while expanding access to specialty care.
Both organizations identify documentation burden as a contributor to clinician burnout. Both also want to expand tele-specialty capabilities so patients don’t have to travel hours to receive specialty consultations.
Each hospital develops an initiative that includes EHR improvements and telehealth expansion.
At a high level, the initiatives are comparable.
But when a state RHT program evaluates proposals, one initiative moves forward while the other does not.
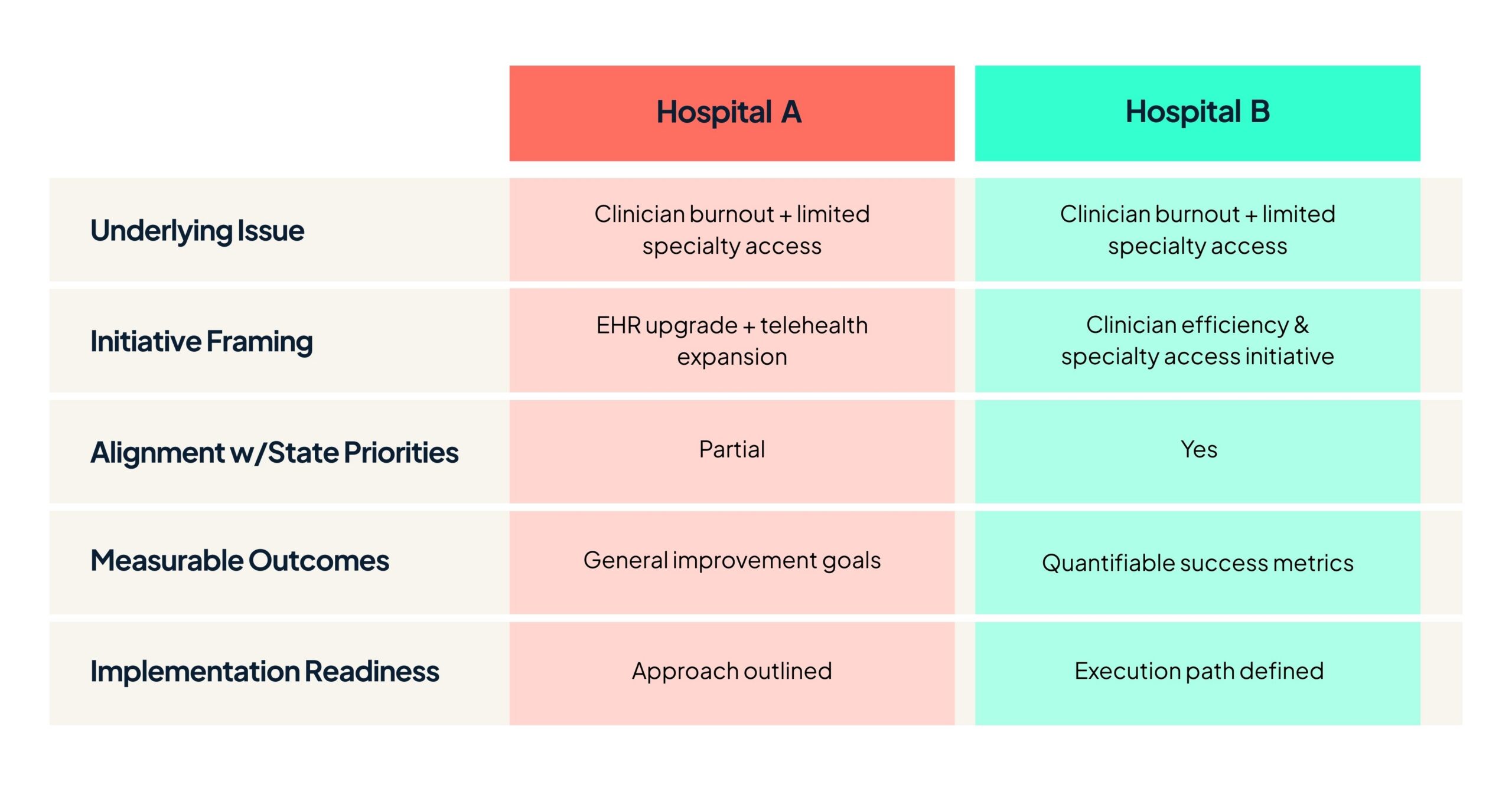
What made the difference?
In many cases, the answer has less to do with the challenge being addressed and more to do with how the initiative fits the framework programs use to evaluate RHT funding decisions.
Where RHT Funding Decisions Actually Happen
RHT funding flows through state-level transformation plans, which then create state-specific RHT initiative categories, collaboratives, or targeted programs that providers can participate in.
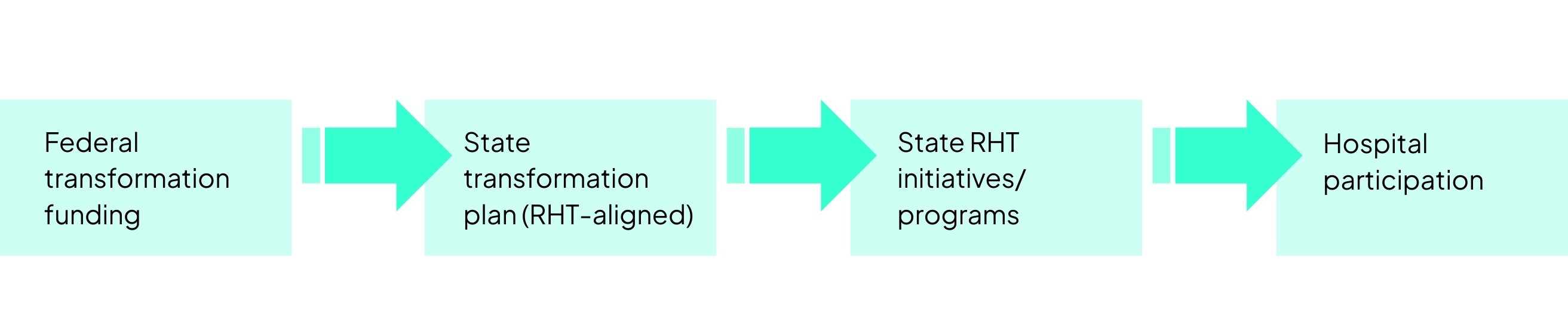
Each state organizes its transformation strategy differently. Some states create a larger number of focused RHT initiatives, while others concentrate funding into fewer programs.
For rural health systems, this means that the structure of state RHT initiatives shapes the opportunity landscape, and hospitals are evaluated based on how clearly their proposed initiatives align with those program categories.
The Framework Behind RHT Funding Decisions
At the federal level, the RHT program is organized around five pillars that define the types of transformation the program is designed to support. While states have flexibility in how they structure their programs, most state RHT initiatives ultimately map back to these five core priorities1:
Make America Healthy Again
Support rural health innovations and new access points to promote preventative health and address root causes of diseases. Projects will use evidence-based, outcomes-driven interventions to improve disease prevention, chronic disease management, behavioral health, and prenatal care.
Sustainable Access
Help rural providers become long-term access points for care by improving efficiency and sustainability. With RHT Program support, rural facilities work together—or with high-quality regional systems—to share or coordinate operations, technology, primary and specialty care, and emergency services.
Workforce Development
Attract and retain a high-skilled health care workforce by strengthening recruitment and retention of healthcare providers in rural communities. Help rural providers practice at the top of their license and develop a broader set of providers to serve a rural community’s needs, such as community health workers, pharmacists, and individuals trained to help patients navigate the healthcare system.
Innovative Care
Spark the growth of innovative care models to improve health outcomes, coordinate care, and promote flexible care arrangements. Develop and implement payment mechanisms incentivizing providers or Accountable Care Organizations (ACOs) to reduce health care costs, improve quality of care, and shift care to lower cost settings.
Tech Innovation
Foster use of innovative technologies that promote efficient care delivery, data security, and access to digital health tools by rural facilities, providers, and patients. Projects support access to remote care, improve data sharing, strengthen cybersecurity, and invest in emerging technologies.
State transformation plans generally translate these pillars into specific initiative categories or programs that hospitals can participate in. When hospitals submit proposals or participate in these initiatives, reviewers are often evaluating how clearly the proposed effort aligns with:
- One or more of the RHT priority areas
- Defined outcomes tied to transformation goals
- The organization’s readiness to implement the initiative
- Governance and leadership accountability
Initiatives that clearly map from hospital proposal to state initiative to RHT pillar are easier for programs to evaluate and prioritize. These are the initiatives that win the most funding.
Why Some Initiatives Fit the Framework Better Than Others
Strong ideas naturally rise to the top, right? Not really.
In practice, state RHT programs evaluate initiatives through a structured lens with defined categories and scoring criteria.
If a proposal does not clearly map to those categories or demonstrate measurable outcomes and implementation readiness, reviewers may struggle to place the initiative within the RHT evaluation framework.
This does not necessarily mean the idea itself is weak. In fact, many unfunded initiatives address real and pressing operational challenges. The difference is often that the initiative is not presented in a way that clearly aligns with how the program evaluates proposals.
In other words, the initiative itself may be similar to one that receives funding, but the structure and clarity of the proposal make it easier for reviewers to say “yes” to.
Translating Operational Challenges Into Initiatives
Check out these examples of how you might re-frame operational challenges as clearly defined RHT initiatives:
Example A
Operational challenge: Documentation burden and EHR inefficiency contributing to clinician burnout
Initiative framing: Clinician Efficiency Initiative; Combining EHR optimization, documentation support tools, and workflow redesign
Why it works for reviewers: Defines a clear transformation effort tied to workforce sustainability rather than a general technology upgrade
Pillars: Rural Workforce, Healthcare Technology
Example B
Operational challenge: Patients traveling long distances for specialty care
Initiative framing: Tele-Specialty Access Initiative; Expanding remote specialty consultations across rural sites
Why it works for reviewers: Frames the effort as a scalable access expansion initiative rather than a telehealth tool deployment
Pillars: Rural Workforce, Healthcare Technology
Example C
Operational challenge: Limited staff capacity for care coordination
Initiative framing: Care Coordination and Digital Patient Engagement Initiative; Combining care coordination workflows, patient communication tools, and remote monitoring capabilities
Why it works for reviewers: Shows how the effort changes care delivery rather than simply adding staff or software
Pillars: Rural Workforce, Healthcare Technology
Example D
Operational challenge: Fragmented data across clinical systems
Initiative framing: Clinical Data Integration and Interoperability Initiative; Connecting clinical systems and enabling shared data for coordinated care and performance reporting
Why it works for reviewers: Positions the effort as enabling coordinated care and reporting, not just technical integration
Pillars: Innovative Care Delivery, Community / Population Health, Healthcare Technology
How Leading Systems Are Approaching the Problem
Because state RHT opportunities are continuing to evolve, many rural health systems are taking a more structured approach to strategy.
Rather than maintaining a wish list of projects, organizations are increasingly organizing their efforts around a small number of clearly defined transformation initiatives with clearly defined ownership, measurable outcomes, supporting tech or infrastructure components, and a clear implementation timeline.
By organizing priorities this way, leadership teams can evaluate emerging RHT opportunities more quickly and determine how their initiatives align with state programs.
Many organizations are formalizing this work through transformation blueprints.
A transformation blueprint helps leadership teams clarify:
- Which initiatives matter most to the organization
- How those initiatives align with RHT priorities and state programs
- The governance and execution structure required to deliver them
- How outcomes will be measured and reported
By organizing transformation efforts this way, rural health systems can present initiatives in a structure that aligns more clearly with how RHT programs evaluate and prioritize proposals.
Preparing for What Comes Next
RHT funding represents an important opportunity for hospitals seeking to address longstanding operational and access challenges. But funding decisions are rarely based on the challenge alone; They depend on how clearly an initiative fits the framework programs use to evaluate transformation efforts.
Organizations that structure initiatives around defined priorities, measurable outcomes, and implementation readiness are often better positioned as new opportunities emerge.
The most well-funded rural health systems develop a clear transformation blueprint as a part of their RHT proposal process.
Quoris builds blueprints that align directly with how states are allocating funds across the five pillars, positioning rural providers to compete for and secure RHT funding, then delivering the technology needed to execute those initiatives.
Share this
